Immune Regulation
Immune Regulation Research
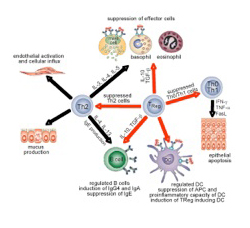
To avoid chronic cell activation and inflammation against nonpathogenic antigens through skin, ingestion, and inhalation, the immune system has developed efficient peripheral tolerance mechanisms. Allergic diseases are caused by an aberrant immune response mediated through a key effector cell, the Th2 cell, and an associated cytokine pattern including IL-4, IL-5, and IL-13. Consequently, the most pronounced findings with potential relevance to allergy therapy are related directly to the control of these Th2 immune effectors. There is strong evidence that peripheralT cell regulation plays a crucial role in the control of harmful T cell responses. Since the early 1970s, many types of suppressor mechanisms have been demonstrated, and the biology of T reg cells has been the subject of intensive investigation. Subsets of T reg cells with distinct phenotypes and mechanisms of action include the naturally occurring, thymic-selected CD4 + CD25 + FoxP3 + T reg cells, and the inducible type 1 T regulatory (Tr1) cells. A great deal of uncertainty remains about differentiation factors, antigen specificity, and mechanisms of action of T reg cells. Several types of adaptive T reg cells have been described with a unique mechanism of action that varies depending on the experimental model. T reg cells act as suppressor T cells, which down-regulate effector cells and APCs in vitro and in inflammation models such as various chronic infections, organ transplantation, allergy, and autoimmunity. Although molecular mechanisms of T reg cell generation remain to be elucidated, some existing therapies for allergic diseases, such as treatment with glucocorticoids and β-2 agonists, might function to promote the numbers and function of IL-10 – secreting Tr1-like cells.

